Here is a really important concept about the SI joint:
How is an SI joint supposed to stay in place?
The body has 2 main systems to maintain stability in the SI joint:
Form closure and force closure.
1) Form closure has to do with the shape of the bones that make up the SI joint (the two hip bones and the sacrum).
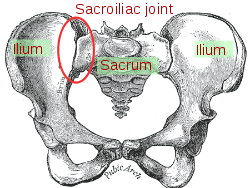
According to Physiopedia, “The sacrum and the ilium each have one flat surface and one ridged surface which interlock together, promoting stability.”
The ridges on each bone serve to create interlocking grooves, which make the joint surfaces “lock” together better. (Or, in more scientific terms, “The symmetrical grooves and ridges allow the highest coefficient of friction of any diarthrodial joint and protect the joint against shearing”).
Everyone has slight differences in the way their SI joints fit together. This difference is greatest between men and women, and also changes across the lifespan. However, even between men or women of the same age, great variation could be found in the shape of the bones making up the SI joint.
Some people’s SI joints will just naturally be more stable, due to the way their bones fit together… and some people’s will be way less stable.
2) Force Closure
Force closure involves the structures of your body that hold the bones of the SI joint together.
According to Physiopedia, these structures include:
- the muscles that cross the area of the SI joint
- the ligaments that hold the bones of the SI joint together
- the thoracolumbar fascia (a big sheet of connective tissue that supports your lower back)
To my knowledge, the thoracolumbar fascia is not something you can have much of an impact on (although there is a lot of new research coming out on it these days!).
Ligaments, also, you cannot have much control over. If a ligament has been injured, it has probably been slightly stretched out, and although ligaments can heal to an extent, there is really no way to make a stretched out ligament completely go back to normal.
You can do things such as rest, to try to reduce inflammation, and there are a few types of injections which doctors can perform to attempt to speed healing (such as cortisone injections and prolotherapy— more on these later). But there is no surefire way to restore a ligament to pristine, pre-injury condition.
The easiest component to have control over is, of course, the strength of your muscles, and also improving coordination. If you’ve had an injury to the SI joint, your muscles have probably been spasming in order to protect the area, which can cause them to become weaker over time. I really recommend seeing a good physical therapist (particularly an aquatic physical therapist) to get some exercises to get these muscles going again.
Sources:
Physiopedia, Sacroiliac Joint Form and Force Closure
The Sports Injury Doctor: Sacroiliac Joint Pain
Diane Lee and Associates: Pelvic Stability and Your Core
Core Concepts: We’ve Heard So Much of the Core, What about the Slings?
Scientific Journal Articles (the heavy stuff):
Van Wingerden, J. P., Vleeming, A., Buyruk, H. M., & Raissadat, K. (2004). Stabilization of the sacroiliac joint in vivo: verification of muscular contribution to force closure of the pelvis. European Spine Journal, 13(3), 199–205. http://doi.org/10.1007/s00586-003-0575-2
Vleeming, A., Schuenke, M. D., Masi, A. T., Carreiro, J. E., Danneels, L., & Willard, F. H. (2012). The sacroiliac joint: an overview of its anatomy, function and potential clinical implications. Journal of Anatomy, 221(6), 537–567. http://doi.org/10.1111/j.1469-7580.2012.01564.x
Kinetic Control: Clinical Notes: Interpretation of modified FORCE CLOSURE model (Mark Comerford MCSP B.Phty MAPA)
Hope this was helpful!