Hi everyone,
I often hear from people who are struggling to tell whether their pain is coming from the SI joint, or another potential cause of low back/hip pain.
I know from personal experience that it can be really overwhelming to try to wrap your mind around exactly all of the things that could be causing your pain.
So here, with illustrations, is a guide of some of the important structures of the pelvis. My goal is to give you a reference to clarify some of the concepts I’ve written about in earlier posts.
(These pictures are all from the front, to keep things in the same orientation. I’ll make another post of views from the back later).
The sacroiliac joint
The sacroiliac joint is formed by the meeting of the sacrum (the base of the spine), and the ilium, or hip bone.
The sacrum:

The ilium (or the hip bone):

And they come together to form the sacroiliac joint:

The Lumbar Vertebrae:
One of the reasons it is so hard to diagnose and treat SI joint dysfunction is that it can be really hard to tell the symptoms apart from spinal issues.
If you look at the picture below, you can kind of see why — the SI joints are so close to the lumbar vertebrae that it’s unlikely that you, as the patient, will be able to tell where your pain is coming from at first. And unfortunately, it probably won’t be obvious to your doctor at first, either.
(Technically the lumbar spine isn’t part of the pelvis, but I’m including it because it’s extremely important to be aware of).
.
That’s why it’s so important to get a thorough evaluation from a physician, to figure out what’s going on.
The Pubic Symphysis
Something else that comes up a lot, when you’re talking about the SI joint, is the other major joint of the pelvis, the pubic symphysis:

Because all of the joints in the pelvis are connected, it’s fairly common to experience pain at the pubic symphysis when you have SI joint dysfunction. When motion at the SI joints is disrupted, motion at the pubic symphysis will likely altered as well, which can create pain, inflammation, and hypermobility..
Here’s a close up:

It’s also fairly common for women to develop pubic symphysis issues during pregnancy or childbirth. It’s also possible for the pubic symphysis is actually the primary source of pain, while the SI joints are unaffected.
For more, check out:
The pubic symphysis: the joint at the front of the pelvis.
My page on Women’s Health also has a few pregnancy-related links which discuss the pubic symphysis as well.
***
The Hip Joint
Another topic that comes up frequently is the hip joint.
The hip joint is where the thigh bone fits into the acetabulum, or the hip socket.
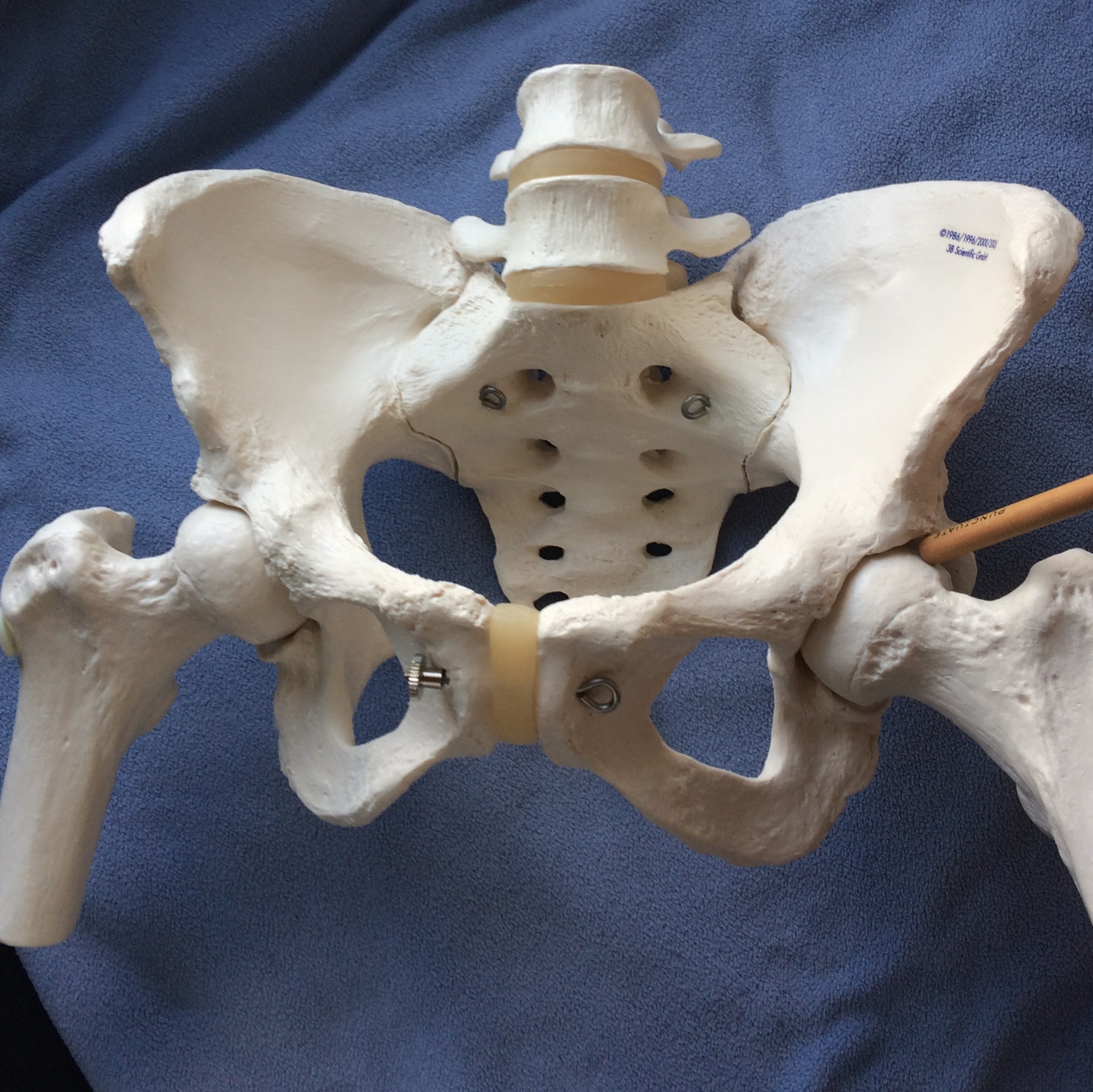
It’s not uncommon to experience problems with the hip joint and the SI joint simultaneously. When you have altered motion in one, it can affect the function of the other.
If your pelvis is rotated out of its normal position, it can change the way your hip joint is oriented relative to the ground. This can lead to short leg syndrome, which means one of your legs will feel shorter than the other, based on the way your pelvis is positioned. (Check out the “Lower Body” section of this post for more).
Labral Tears
If you subject your hip joints to abnormal wear and tear, this can also create problems with the ring of cartilage inside of the hip socket, which is known as the labrum. You can develop inflammation or even a tear in that cartilage, known as a labral tear.
I was lucky to never experience one, but the two issues can go hand in hand.
Here’s a close up of the hip socket (the acetabulum):

The only cartilage shown on this model is at the pubic symphysis, however the labrum would be a ring inside of the hip socket, cushioning the top of the femur (thigh bone).
For more on the hip joint, you can check out:
***
The Femur (Leg Bone)
The femur of course, is not technically part of the pelvis either, but it’s still very much relevant here.
My model obviously only has the top part of the femur, but you can still get a good idea of how it fits into the hip joint.
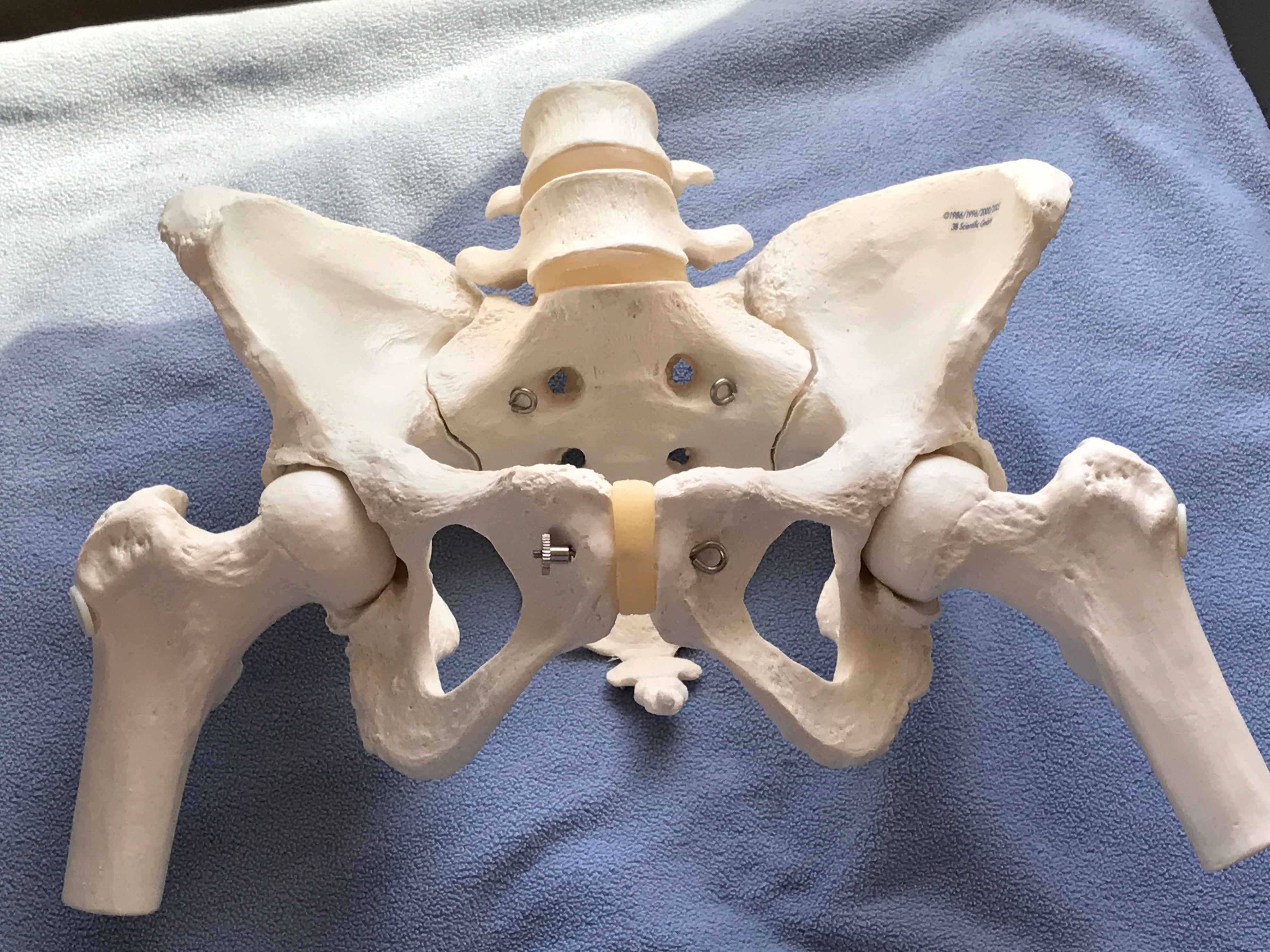
I once heard from a reader who was suffering from trochanteric bursitis along with SI joint dysfunction. The greater trochanter is the name for that big round “knob” that sticks out of the top of the femur. Its purpose is to serve as an attachment point for a lot of major muscles.
If you have bursitis, it means you have inflammation in some of the protective “pads” the body places over that bony knob, to protect it from impact. In the case of trochanteric bursitis, it means you have inflammation of the bursa right over the greater trochanter.
SI joint dysfunction can indirectly lead to this, by creating abnormal movement patterns and muscle tension that put a lot of stress on that area.
***
everything is connected
So as you can see, everything in the body is connected. An issue or dysfunction in one part of the body can lead to an issue in another. However, it is possible to sort it all out– sometimes it just takes time, consistency, and dedication.
***
So… wow, that was quite the textbooky post, so that’s all for now. I hope these images were useful and helped clarify how some of these structures relate to each other. Any questions, feel free to reach out!
Christy,
You have described the kinetic chain so clearly. These parts are so closely connected it is no wonder when something becomes injured it affects so many other things. Muscles, nerves, ligaments, bones all working together. It is a puzzle indeed!
LikeLiked by 1 person
Absolutely! I’m so glad you found the post helpful.
LikeLike
Is the kinetic chain the reason I seem to benefit more from rehabilitative group exercise classes than private sessions? I’m wondering if the “stop and go” nature of private sessions impedes rather than helps the functioning of the kinetic chain. I always feel better after a group class, and the only reason I can think of is that the movement is continuous.
LikeLike